by Riley Voss and Brantley Scott
Trends in prescribing practices and emergency room visits decreased in Utah during 2017-2020 despite the opioid epidemic wreaking havoc throughout the country (figure 1). This may be attributable to the variety of public health interventions and increased resources [1,2]. According to the Utah Department of Health and Human Services’ media campaign, Stop the Opidemic, five Utahns die every week from opioid overdose [3]. The Centers for Disease Control and Prevention estimate that the economic burden of prescription opioid misuse costs roughly $78.5 billion annually in medical costs, productivity loss, treatment for addiction, and criminal justice costs [4]. The National Institute of Health defines opioids as a class of drugs that interact with opioid receptors on nerve cells in the body and brain [5]. Common opioids include prescription pain relievers such as oxycodone, hydrocodone, codeine, and morphine, as well as synthetic drugs like fentanyl, and illegal drugs such as heroin [5]. Prescription opioids, if used properly, can be a safe and effective pain reliever for acute pain but they have a high potential to be dangerous due to the euphoric effect it has on users, which increases the risk for developing dependency, abuse, addiction, overdose, and death [5]. In 2020, there were roughly 1653 opioid related emergency department visits and 357 opioid related deaths in Utah [6].
To further observe the effects of the opioid epidemic and related overdoses in Utah, the Healthcare Information and Analysis Programs conducted an analysis using the Utah All Payer Claims Database (APCD) [7] and the Utah Healthcare Facilities Database (HFD) [8]. The APCD includes medical and pharmacy claims from Medicaid, Medicare Advantage, and qualifying commercial insurance carriers. Claims for approximately 70% of Utahns are included in the APCD. The Healthcare Facility Database contains encounter records for all licensed hospitals, emergency rooms, and ambulatory surgery centers in Utah. These data represent all hospitalizations, emergency department visits and ambulatory surgeries and diagnostic procedures performed in Utah regardless of payer. The records contain information about providers, patients, and billed charges. APCD claims data from 2017-2021 were used to determine the number of opioid prescriptions per person as well as the number of pills per prescription. Emergency room counts and demographics were obtained from the HFD. Overdoses were classified into the opioid, heroin, or methamphetamine categories by looking at the first three diagnosis codes entered for patients’ emergency department visits. A complete list of the ICD diagnosis codes used is stored here:
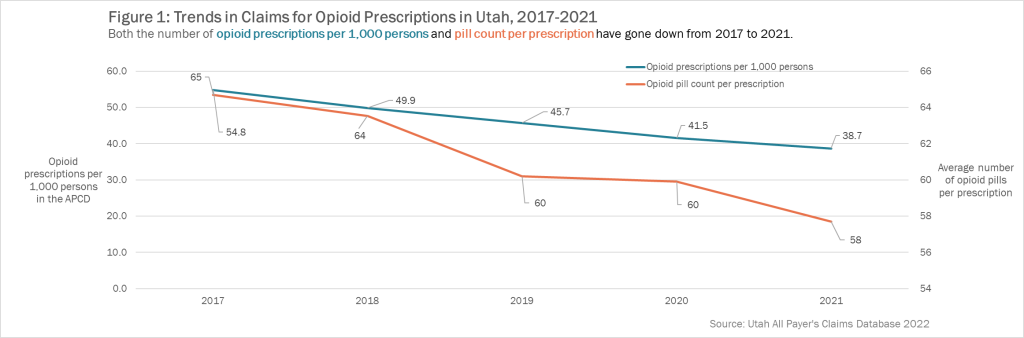
In recent years, there has been an increased awareness of over-prescribed opioids as well as increased action to reduce excessive prescribing practices [4] . Efforts such as provider detailing which includes education from pharmaceutical companies and manufacturers to prescribers about the best prescribing practices and risks of overprescribing opioids [9]. The goal of these programs is to create behavioral change among physicians, pharmacies, and other prescribers to decrease unnecessary prescribing [9]. The effects of these programs have resulted in a decrease of prescribing opioids in Utah, which can be seen in Figure 1 [2]. Figure 1 shows the number of opioid prescriptions per person in the APCD as well as the average number of opioid pills per prescription, both of which have shown a decreasing trend since 2017.
While the opioid epidemic has spread throughout the country over the last several decades, there has also been increased efforts to combat and prevent opioid abuse. Some notable interventions found in the United States include targeted naloxone distribution, medication-assisted treatment, fentanyl screening, good Samaritan laws, and academic detailing [9]. Such interventions have helped decrease misuse, overdose, and emergency room visits, as demonstrated in Figure 2.
Figure 2 shows the number of opioid-related emergency room visits per Utahn due to opioid poisonings including prescribed and illicit substances. Poisonings by heroin, opioids, and methamphetamine have shown a decreasing trend since 2017.
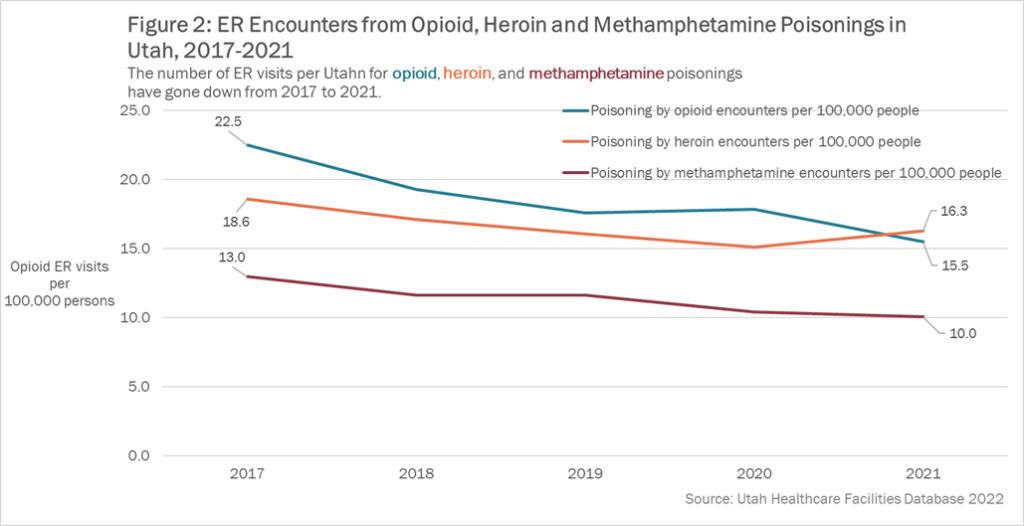
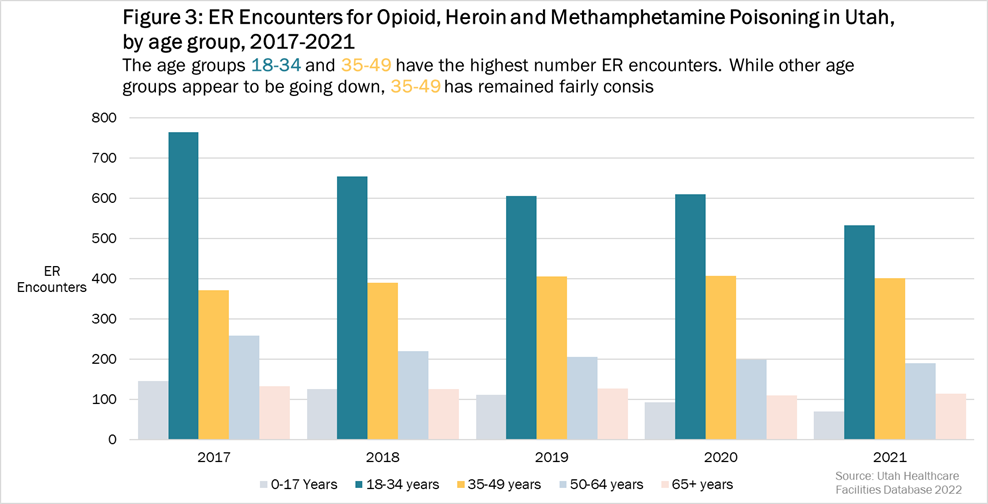
Figure 3: Emergency room encounters from opioid, heroin, and methamphetamine poisoning in by age group, Utah, 2017-2021. The age groups 18-34 and 35-49 consistently had the highest emergency room encounters while other age groups decreased during 2017-2021.
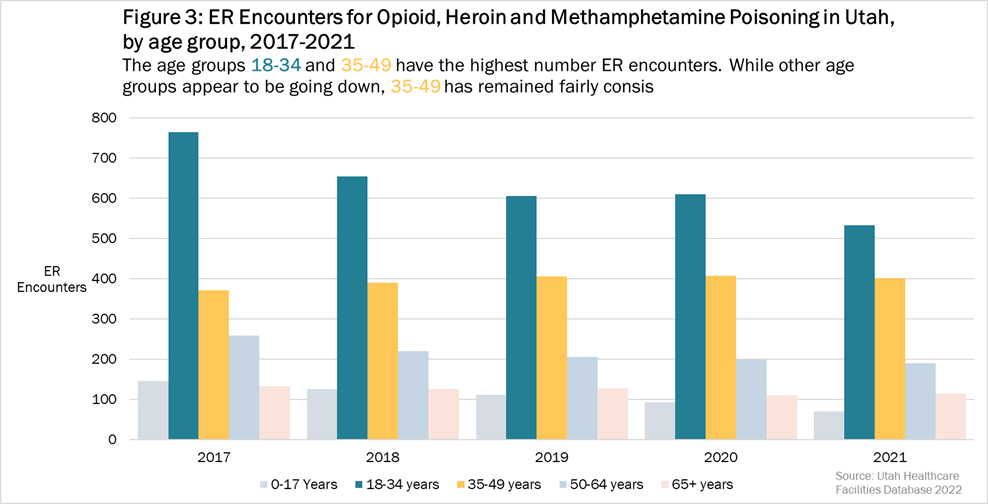
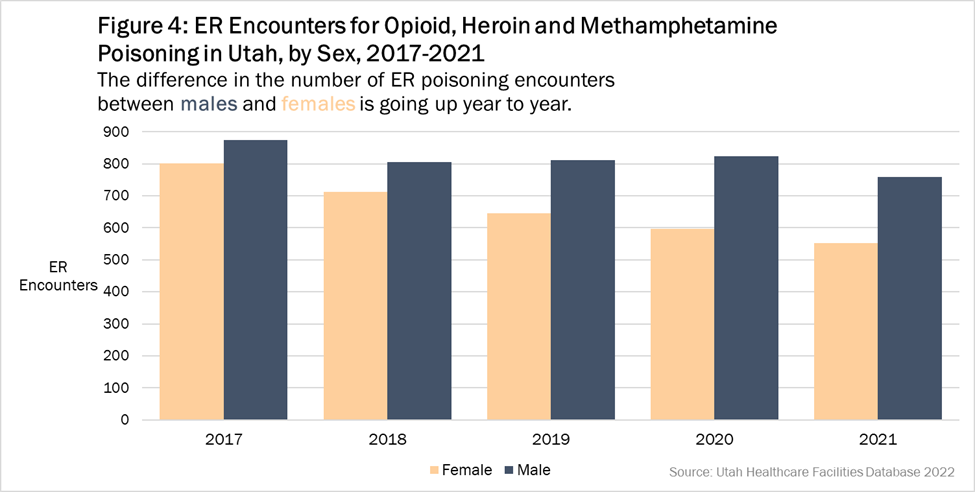
Figure 4: Emergency room encounters from opioid, heroin, and methamphetamine poisoning, by sex, Utah, 2017-2021. Emergency room poising encounters have decreased among women and remained consistent among men from 2017-2021.
While the opioid epidemic continues to affect Utahns, the decreasing trends in prescribing and emergency room visits show that interventions across the state may be preventing abuse and providing effective resources. Meghan Balough from the Utah Department of Health and Human Services Violence and Injury Prevention Program states:
“while the number of prescription opioids dispensed has continued to trend downward for the last several years, prescription opioids are still the most common opioid involved in drug overdose deaths in Utah. We must continue our efforts to educate prescribers, pharmacists, and patients alike regarding the dangers of prescription opioids. By educating the population on alternative therapies, safe prescribing practices, and safe storage/disposal of these medications, we can continue to see decreases in prescription opioid overdose deaths.”
The trends observed from this analysis sheds light on the progress being made in Utah to address the opioid epidemic.
To learn more information about opioids and access resources for help, visit the following websites:
- Opidemic https://www.Opidemic.org
- CDC: Get Informed https://www.cdc.gov/rxawareness/information/index.html
- Utah Naloxone program http://www.utahnaloxone.org/
- CDC: Save a Life https://www.cdc.gov/rxawareness/prevent/index.html
- CDC: Recovery is Possible https://www.cdc.gov/rxawareness/treatment/index.html
[1] https://physicians.utah.edu/echo/clinical-support-areas/substance-use-disorder [2] https://academic.oup.com/painmedicine/article-pdf/12/suppl_2/S73/5411217/12-suppl_2-S73.pdf [3] https://www.opidemic.org/ [4] https://nida.nih.gov/research-topics/opioids/opioid-overdose-crisis [5] https://nida.nih.gov/research-topics/opioids [6] https://vipp.health.utah.gov/opioid-overdoses/ [7] https://healthcarestats.utah.gov/about-the-data/apcd/ [8] https://healthcarestats.utah.gov/about-the-data/healthcare-facility-data/ [9] https://www.cdc.gov/drugoverdose/pdf/pubs/2018-evidence-based-strategies.pdf