By Brantley Scott
In the healthcare industry, two of the things that Utah is well known for are: having a healthy population and a high birth rate. However, Utah healthcare needs and risk are not homogeneous. In this DataByte we look briefly at the different maternal risk scores by county and by payer type, Commercial and Medicaid. We will also look at how complications of delivery impacts the healthcare costs.
The risk score calculation in this DataByte uses the Milliman Advanced Risk Adjuster (MARA) medical concurrent model for the 2018 data year. These scores have been normalized to Utah’s entire All Payer Claim Database (APCD) population, which means a risk score of 1 represents average risk and a risk score of 2 represents double the average risk.
As we begin looking at maternal risk in Utah we will first look at the risk scores of the combined pregnant population. The average county risk is 1.7 with a high of 2.1 (Wayne) and a low of 1.2 (Kane). The standard deviation of this population is 0.205.
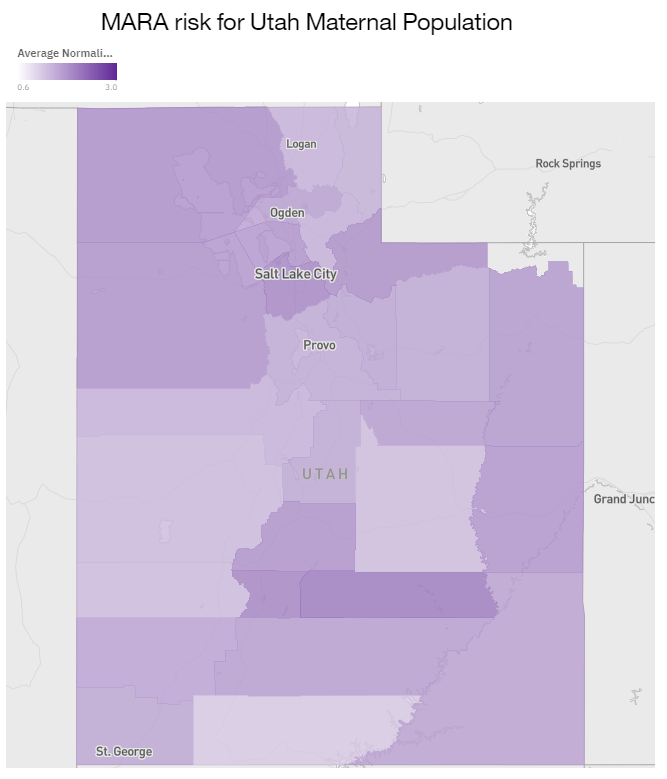
The risk scores start looking more interesting when we separate the commercial and the Medicaid population. For the commercial population the average county risk is 1.5 with a high of 1.9 (Summit) and a low of 1.2 (Kane, Emery, and San Juan). While the Medicaid population’s average is 2.0 and has a high of 3.0 (Garfield) and a low of 1.2 (Beaver). What is even more interesting is the differences in variation. The commercial population only has a standard deviation of 0.162 while the Medicaid population is more than double at 0.379. This indicates that there is a greater geographical impact on the Medicaid population than the commercial population.
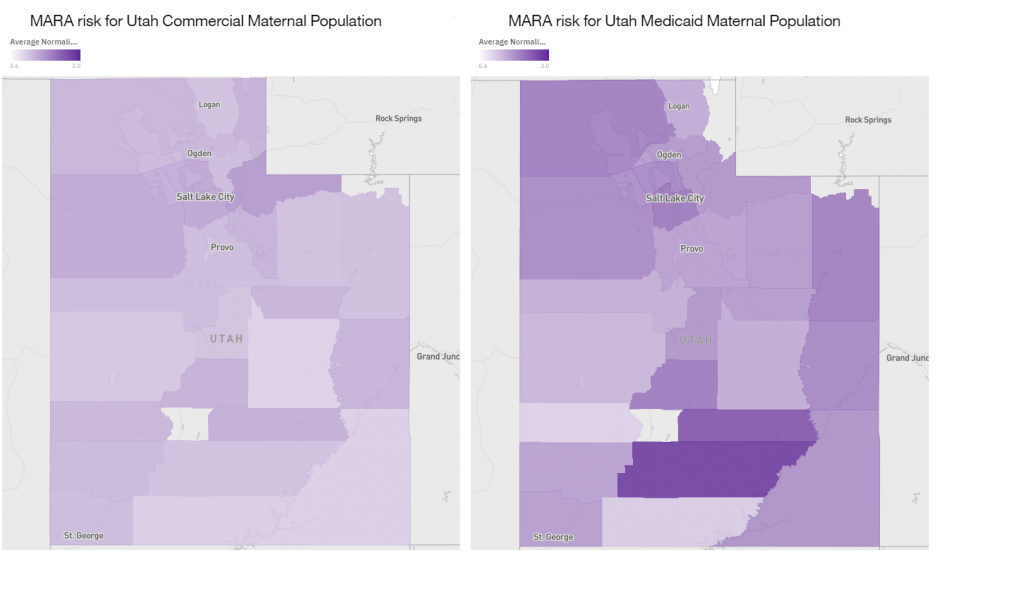
We now change our attention to the financial impact high healthcare risk can have. Having a healthy pregnancy and uncomplicated delivery has significant ramifications for the family, both emotionally and financially. Although our data does not capture the emotional toll a complicated pregnancy and delivery has on the family, we can examine the financial cost of that delivery.
For this analysis we used the MS-DRGs for cesarean (765 & 766) and vaginal (774 & 775) deliveries. Although a delivery usually has multiple healthcare cost components (including OB/GYN costs, costs incurred for the baby, and facility costs), for simplicity we looked solely at the facility costs. Using the 2017 inpatient data from Utah OpenData we estimated the 25th, 50th, and 75th percentile for the above mentioned MS-DRGs.
| MSDRG | Description | 25% | Median | 75% |
|---|---|---|---|---|
| 775 | Vaginal Delivery w/o Complicating Diagnoses | $4,810 | $4,820 | $6,039 |
| 774 | Vaginal Delivery w/ Complicating Diagnoses | $5,424 | $5,754 | $7,247 |
| 766 | Cesarean Section w/o Complicating Diagnoses | $7,714 | $7,729 | $9,745 |
| 765 | Cesarean Section w/ Complicating Diagnoses | $9,208 | $9,226 | $11,766 |
Individual maternity costs will vary by plan design and facility, but these estimates highlight that as complexity of delivery increases so does the associated cost.
This DataByte shows that there are geographic and payer type maternal healthcare risk disparities in Utah. Further research is needed to better understand what is driving these differences and what can be done to improve the health of Utahans’ everywhere.